Every day, 13 people die waiting for a kidney transplant. A mother of three wasn’t going to let that happen to someone in her own family.
6:21 a.m.
Donating a kidney isn’t exactly like lending someone a pencil.
It involves risk. Sacrifice. Guts.
Tara Hansen has always had guts. As a teenager, Hansen pierced her own belly button with a horse needle she bought at a farm supply store. Older now, but no less stubborn, the 31-year-old mother of three said she had a “weird feeling” as soon as she found out that her cousin needed a kidney.
”Watch,” she said. “It’ll be me.”

On a frigid January morning, the gathering of two families in the lobby of Intermountain Medical Center in Murray is evidence that she was right.
J.C. Lay, her 26-year-old cousin, has something called Alport syndrome. The rare genetic disorder has stalked his family for generations. Mothers carry it; sons get it.
Lay’s Uncle Joseph was 2 years old when Lay’s grandmother noticed his urine was the color of Coca-Cola. Joseph’s brother, Jeremy, was also diagnosed with Alport syndrome later.
By the time Lay was born, everyone knew how it would play out: Without the genes necessary to produce a certain type of collagen, his eyesight and hearing would go first. Then, as the disorder started to warp the lining of his kidneys, waste would build up in his blood. Eventually, Lay would go into kidney failure.
Maybe because it made his dad so anxious, Lay tried not to worry. He set out for his mission for The Church of Jesus Christ of Latter-day Saints in Spokane, Washington, at 19 years old. But even then tests revealed his kidney function was down to 68 percent.
He returned home in 2011 and started dating his future wife, a girl named Stephanie, whom he had known since childhood. They got married. He started school. They had a baby.
By May of 2015, things had accelerated. With his eyesight and hearing worsening, Lay’s kidney function dropped to 22 percent. He lost weight. He lost focus. His skin turned ashen. His eyes, already brown, seemed almost black.

A month later, doctors were startled to learn his kidney function had dropped to 6 percent. He would have to go on dialysis immediately.
Lay was 25 years old. His son, Hendrix, was 3 months old.
At home, Lay’s father cried. Uncle Joseph got a kidney transplant when he was 40; Uncle Jeremy when he was 33.
”I thought we had 10 years to do this,” Cole Lay shouted.
During a surgery to put a dialysis port in Lay’s stomach, he vomited several times. Lay’s dad and cousin carried him from the car to the house, his thin arms draped around their necks, his head hanging to the side.
”This kid was just lifeless,” said Lay’s aunt, Tami Hess. “Watching all of that, I was just going, ‘Twenty-five? We’re going to do this at 25?’ You’d watch him and you’d just think, ‘How long can you do it?’”
On the morning of the surgery, Hess grasps her daughter’s arm. They’re wearing the same silver nail polish. Even now, they worry that something could go wrong. That the doctors could call the whole thing off.

7:30 a.m.
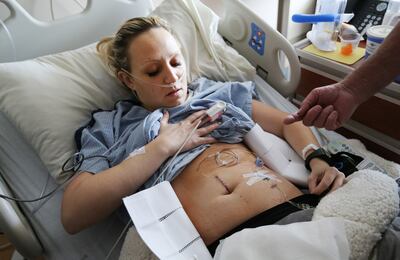
Nurses place Lay and Hansen in prep rooms next to each other.
The two are cousins but feel more like brother and sister. Other than Lay’s mission, the two have never lived more than a few minutes apart. Hansen was the older sister figure, the babysitter who would chauffeur Lay and her little brother around St. George. On weekends, the three cousins would swim, play basketball and fight.
”His mom would always yell at us to stop because of his kidney,” said Hansen’s little brother, DJ Tischner.
Still, nobody could have predicted that Hansen would be the one to donate a kidney. Tischner had always been closer to Lay. But he turned out to be the wrong blood type. Lay’s dad, Cole, also struck out — kidney stones.
But Hansen was passing all the tests. The transplant team put her through a battery of them: Blood tests. Psychological evaluations. X-rays. MRIs.
Her mom and dad fretted. Their family has its own history with kidney disease.
Hansen’s beloved grandfather, Don, was a decorated basketball coach whose kidneys started failing when he was in his 70s. Three times a week, he would wake up at 5:30 a.m. to go to the dialysis center — an exhausting treatment that left him cold, nauseated and too tired to do much of anything.
“That final day, he said, ‘I’m not going anywhere,’ and he didn’t wake up,” Hess said. “To me, when people talk dialysis, I just get so sick to my stomach.”
Doctors warned Hansen about the risks involved, including the possibility of complications during surgery. No aspirin for the rest of her life. No risky sports like skiing, snowboarding or rock climbing.
Then another reality kicked in: When Hansen realized she wouldn’t have an extra kidney to give one of her kids in case they needed one, she cried.

The transplant team told Hansen she could back out whenever she wanted. Even if it was the day before. Even if she was being wheeled into surgery and got a bad feeling all of a sudden.
Her parents asked her if she was sure. “I can deal with other stuff,” said Hansen’s father, Jerry Tischner, a former fire captain. “But not when it comes to your own kids. … You’re programmed not to let them get hurt.”
Hansen was immovable. That was her: strong-willed, fiercely protective, generous to a fault.
In the prep room, Dr. Shiro Fujita, a surgeon, comes to check on Hansen. He warns her that Lay will likely wake up from surgery feeling amazing. Hansen, having lost an organ, will probably feel awful.
She’s unfazed.
”Maybe in my life there’s going to be other reasons,” she said. “But other than raising kids to be great humans and to do big things themselves, I think this is what I was meant to do.”
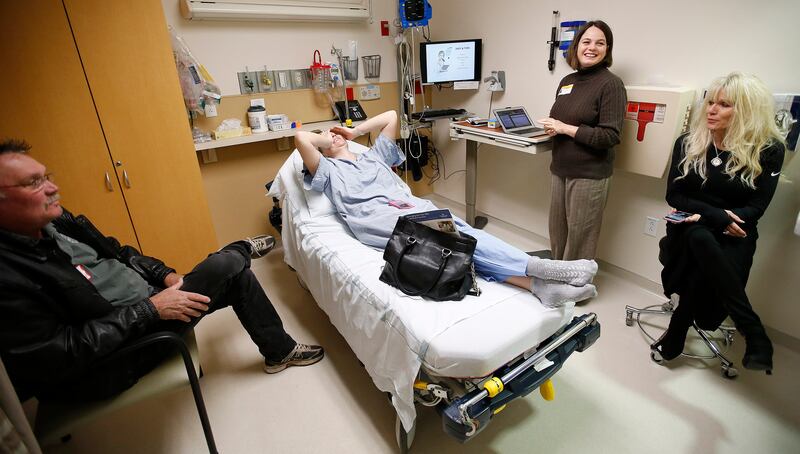
8:01 a.m.
Lay’s stomach hurts, and he’s dying for a bowl of cereal.
He hasn’t eaten anything in 24 hours in preparation for today, a day when absolutely everything has to go right.
Although his health insurance paid for most of the transplant itself, one of the biggest concerns was how the young couple would pay for his other expenses, like medication, travel and dialysis.
In the end, it was the small communities of southern Utah that came through.
DJ Tischner, who is in fact a DJ, spread the word on his radio show. Listeners began to donate. Callers chipped in. Hess held a fundraiser in St. George.
In small-town Milford — where Lay’s parents-in-law have ties — residents held a raffle for Lay and gave away a gun as the prize.
In Paiute County, where Lay’s grandparents are from, three small communities organized a rodeo and passed around a donation bucket.
And it wasn’t just money. People prayed. Strangers called. Then they started signing up to donate their kidneys.
“(The transplant team) said they’ve never had so many people in the donation process,” DJ Tischner said.
”I had someone call me on the phone who I never thought would call me on the phone and they said, ‘Cole, I want you to know, if you need any money at all, you just call me,’” Lay’s father said.
Lay, now tethered to a dialysis machine at home while Hendrix was learning to walk, started to feel hopeful.
“I can’t imagine being alone and going through something like this,” Lay said. “You need that support system — people to lean on and encourage you to get better and have a positive outlook.”
Back at the hospital, Hansen shuffles over to Lay’s room to give him a final kiss on the forehead.
He hugs her back.
They are both a little nervous.
”Poke him hard,” she tells the nurse. Then they’re wheeling her out of the room and into surgery.
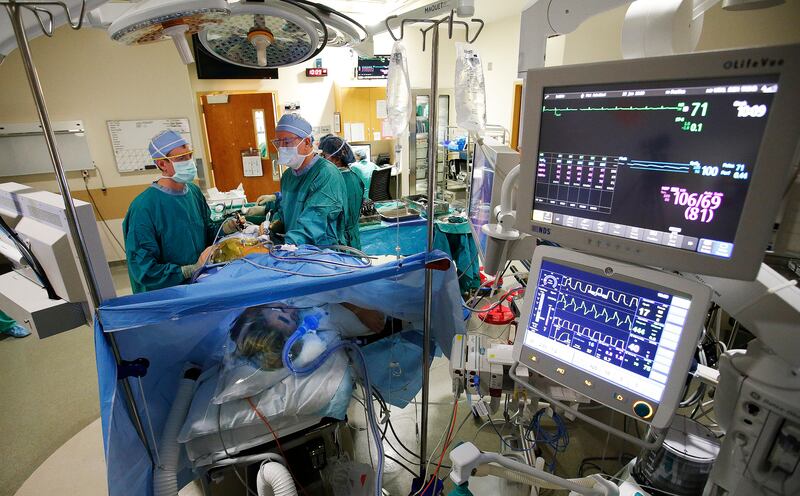
9:23 a.m.
Hansen’s body, protected under a blue tarp, seems too small for the cavernous operating room.
Her abdomen is a yellow square, framed under glaring lights.
Using a pair of electrosurgical scissors, Dr. Willem Van der Werf cuts away at the tissue around Hansen’s kidney. He works through an incision in her abdomen, using a tiny camera to see what he’s doing. With each painstaking snip, the camera captures a burst of molecules fizzling into the air: vaporized tissue.
For those who work in the operating room, transplants are often the best part of the job.
”We deal with a lot of really negative things,” said registered nurse Michael Sherer. “I love doing (transplants) because of the positive outcome at the end of it. It gives you a completely different outlook on life.”
It’s uncommon for someone like Lay to find a kidney donor within a matter of months. Kidneys are the most sought-after organs in the U.S. Nationwide, the average wait time to get one is 3.6 years.
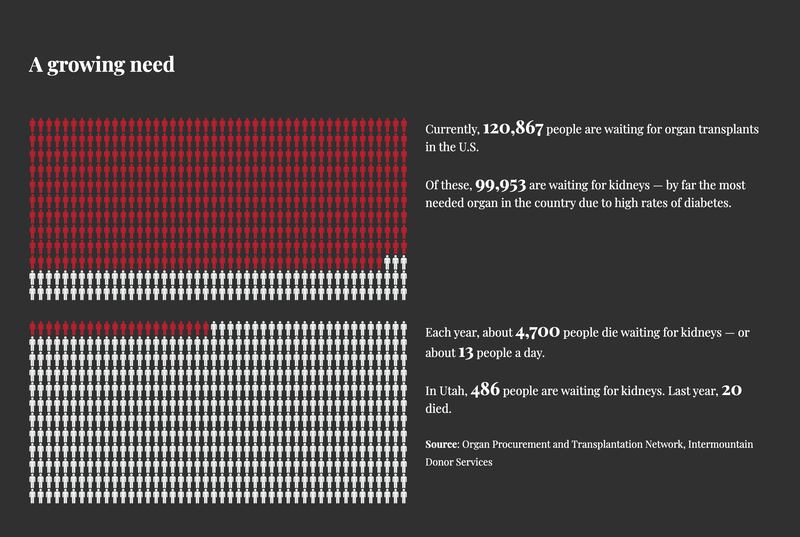
If enough people signed up to be donors, the waitlist could easily be eliminated, said Dixie Madsen of Intermountain Donor Services. But it’s been challenging for organ procurement organizations to raise awareness and overcome peoples’ fears about live organ donation.
“It’s a very disheartening situation when someone passes away on the waiting list because you know that, technically, their life probably could have been saved,” Madsen said.
Unfortunately, many patients don’t have a family member or friend who is a match.
Intermountain Donor Services tries to help by organizing kidney donation chains and promoting its Good Samaritan kidney donation program, which matches volunteers with recipients. Since being founded in 2002, 80 volunteers have successfully donated their kidneys to strangers, according to Madsen.
“When you talk to people who have done that, it’s kind of amazing, because their response is, ‘If I had another kidney, I’d do it again in a heartbeat,’” Madsen said.
Nationwide, about 55 percent of people are registered to be organ donors. In Utah, the percentage is even higher, at 78 percent, according to Madsen. Still, the waitlist grows longer every year.
“There’s just not enough organs to keep up with the demand,” Madsen said. “We need more than 55 percent nationwide to be able to do that.”

11:28 a.m.
After two hours of surgery, Van der Werf comes to the most dangerous part of the operation — separating Hansen’s kidney from her artery without nicking it and causing uncontrollable bleeding.
A bowl of ice, which an assistant has been stirring occasionally for the past two hours, awaits Hansen’s kidney.
The bags of bloody towels have piled up.
Fujita waits impatiently by Van der Werf’s side.
Every minute counts.
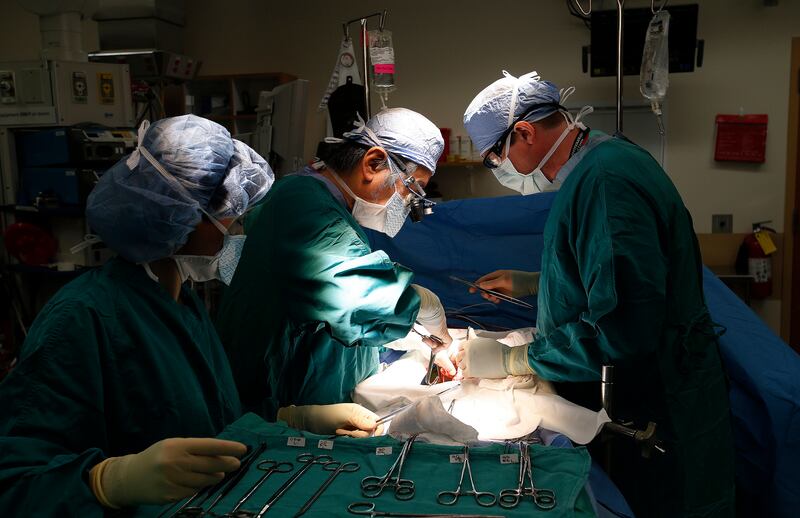
11:49 a.m.
Fujita dashes out of the doors and into the neighboring operating room.
He works quickly to clean Hansen’s kidney — a firm, pale, bean-like thing.
Pulling veins this way and that, Fujita goes about the delicate task of undoing the staples and clips that Van der Werf used to stem the flow of blood in Hansen. He will need to reconnect Hansen’s kidney to Lay’s blood vessels.
As an assistant hands him needle and thread, Fujita prepares to place the kidney inside Lay’s abdomen.
He works with complete concentration.
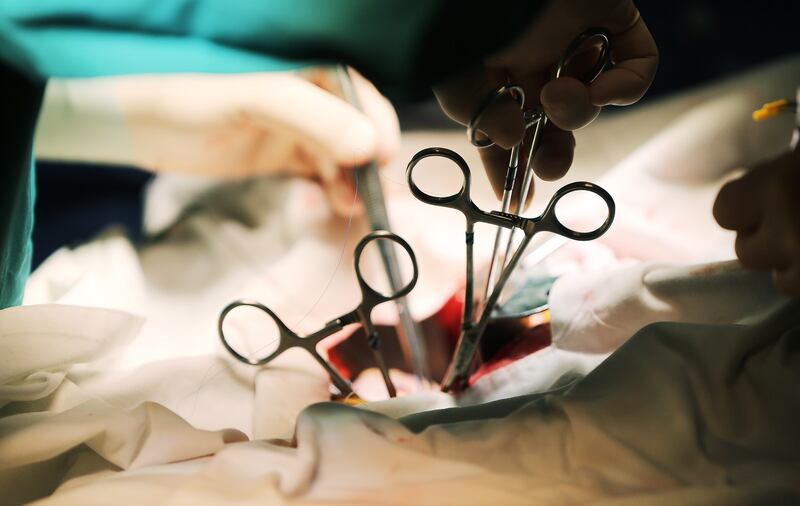
12:54 p.m.
As Lay’s blood starts pumping through Hansen’s kidney, the organ flushes and turns pink.
It’s working.
A new day
Lay was able to walk first. He made sure to stick his tongue out at Hansen as he passed by her room.
”That’s a good kidney you got there, buddy,” Hansen reminds him.
For days, all they do is inch along the hallways on the 10th floor, leaning on their IV stands for support. They’re part of a procession of patients who have had surgeries on their knees, hips and hearts, learning to walk again after being cut open.
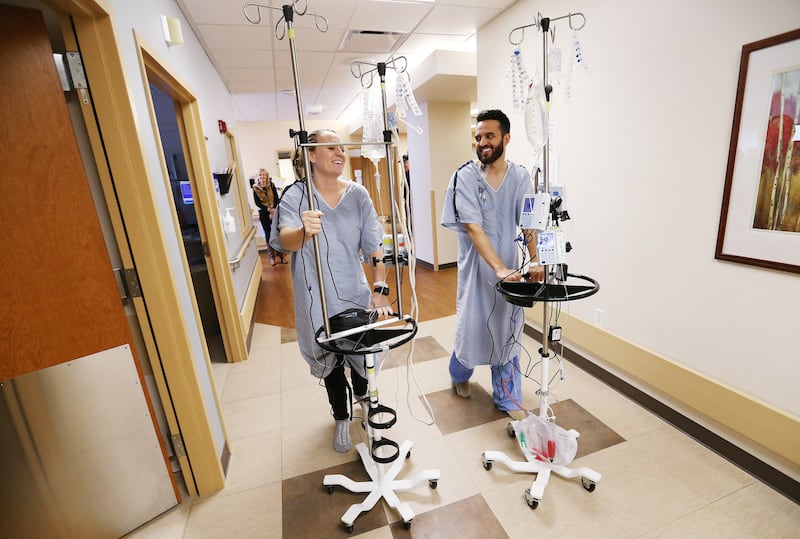
Lay’s body will fight the kidney for the rest of his life. In 15 to 20 years, he’ll probably need a new one.
Tubes are sprouting out of a 10-inch scar on his abdomen, stapled together like a sideways grin.
Two months later, Lay’s Frankenstein scar has faded to a crooked smile.
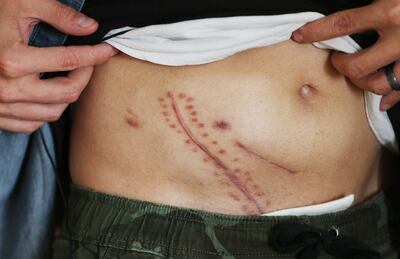
Alport syndrome will continue to attack his family. The next person to need a transplant is likely Lay’s 20-year-old cousin, Wyatt Smith.
“I think he’s scared about it, but he doesn’t want to admit that,” said RaeDawn Smith, his mom. “It’s tough, but I just tell him that we can’t worry about it until we have to worry about it.”
She was scared when Lay’s kidneys started failing so early, but so far, Wyatt hasn’t shown any signs of kidney failure, she said.
”I don’t want (Wyatt) to go through dialysis,” Smith said. “I don’t want him to have to go through this at all.”
Because Alport syndrome is a rare disorder — affecting fewer than 1 in 5,000 people — it is unlikely that any pharmaceutical company will invest in finding a cure. Hearing loss remains a big problem for people with Alport syndrome, and their stories almost always end in dialysis and transplantation.
But in Lay’s words, tough times become “a magnetic field for miracles.” Because of the experience, many members of the family say their idea of sacrifice has changed.
“There was nothing in it for (Tara),” said Cole Lay. “Everyone says they will, but when it gets time to do it …” He trails off. “Tara, I can’t believe it. She didn’t flinch.”
After getting back to St. George, Hansen waited three weeks before going back to work at a mortgage company. Shortly thereafter, she returned to the gym. Now she’s participating in a weight loss competition.
”I don’t like when people say ‘You saved his life’ or ‘You’re an angel’ or ‘You’re a hero,’” Hansen said recently. “I get uncomfortable with it because I don’t feel like I am. I don’t feel like I did anything special at all. It was just something I know I was meant to do.”
Her kidney — now Lay’s kidney — is functioning better than anyone expected. Lay wakes up early, works a full day, takes care of Hendrix and plays tennis with his wife.
Now that the transplant is over, they keep joking about getting a “sweet kidney tattoo.”
But Lay said he doesn’t need ink to remind him of his everyday angels — the people who stuffed bills into donation jars, stitched healing threads through his body or simply carried him when he was too sick to stand.
Doctors say that when Lay’s swelling finally goes down, he’ll be able to put his hand on his belly — right on his hip — feel the kidney pumping.
“Having Tara make that sacrifice,” Lay said, “is something that’s always going to stay with me.”

