SALT LAKE CITY — In a nation that is steadily growing fatter, Utah remains an outlier of relative good health, with an obesity rate that ranks among the lowest in the nation, especially when it comes to children, according to a report released Thursday.
But that’s no cause for celebration with an extra helping of dessert because Utahns are also gaining weight, just not as much as the rest of the nation, according to the annual “State of Obesity” report produced by the Trust for America’s Health.
Nine states now have obesity rates higher than 35%, and more than half of adults in every state are either overweight or have obesity, the report said.
While at 27.8%, Utah’s obesity rate is significantly lower than Mississippi and West Virginia, where the rate is just under 40%, obesity is on the rise in the general population, with the obesity rate increasing by more than 15% since 2013.
“These latest data shout that our national obesity crisis is getting worse,” said John Auerbach, president and CEO of the Trust for America’s Health. “They tell us that almost 50 years into the upward curve of obesity rates we haven’t yet found the right mix of programs to stop the epidemic. Isolated programs and calls for lifestyle changes aren’t enough.”
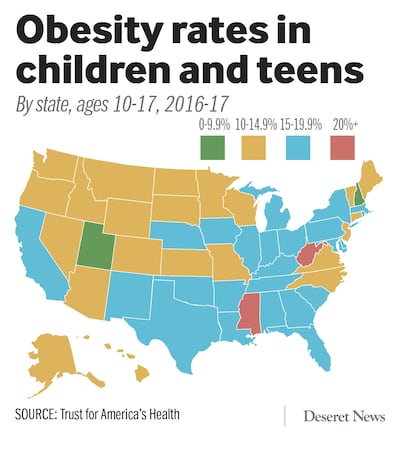
But there are stark geographical differences in obesity, the report found.
Led by Colorado, the states with the lowest obesity rates cluster in the West and mountain states, and in New England.
And Utah and New Hampshire are tied for the lowest obesity rate among children ages 10-17.
The distribution shows that America is not only divided along political lines, but also in matters of health. Obesity’s prevalence corresponds with poor outcomes in a variety of markers, including disease and longevity. And since rates are highest among minorities and the poor, policymakers should aggressively seek solutions, including taxes on high-sugar drinks, expanded nutrition programs for the poor and initiatives to encourage physical activity, the report said.
They could also look to Utah and other states with historically low rates to see what they’re doing right.









The latest numbers
As recently as 2012, no state had an adult obesity rate over 35%; now, nine states do, including Kentucky, Missouri and North Dakota, the three states new to the list.
Inching closer to that is the national obesity rate, which stands at 30.9%, the report said. That means that about 1 in 3 Americans have obesity, which the report authors say is an “extraordinary” jump over the past 30 years.
Surveys conducted between 1988-1994 and 2015-16 found that the rate among adults increased more than 70% and by 85% among children.
Historically, Utah has ranked among states with the least obesity, and this year, at 27.8% it is about 3 points below the national average and ranks 40th in the nation. But Auerbach cautioned that state health officials shouldn’t be too jubilant about that, given that Utah is among six states that saw a 15% or more increase in obesity between 2013 and 2018. (The others are New Mexico, Nebraska, Minnesota, Missouri and Florida.)
“Utah, while better than so many other states, is still feeling the impact of this national — one could say global — trend of consumption of unhealthy foods, reduction of physical activity, and, as a consequence of that, significantly poorer health,” Auerbach said.
The health consequences of obesity include an increased risk for Type 2 diabetes, high blood pressure, stroke and many types of cancers. Obesity is estimated to increase national healthcare spending by $149 million annually (about half of which is paid for by Medicare and Medicaid), and being overweight or obese is the most common reason young adults are ineligible for military service, the report said.
Obesity is also blamed, in part, for the recent declines in life expectancy in the U.S.
Of particular concern in Utah, Auerbach said, are diabetes and hypertension, which are more likely to afflict people who are significantly overweight.
“There, too, Utah is better than most other states, but 8% of the adult population has diabetes, which is the No. 1 cause of blindness, amputation and kidney failure. Diabetes, Type 2, numbers track almost exactly to obesity,” Auerbach said.
“And 1 in 4 adults in the state have hypertension, which can lead to all kinds of very significant health risks to the adult population,” he said.
What Utah does right
Obesity is more prevalent among minorities and people with lower incomes.
Nearly half of Latino (47%) and black adults (46.8%) had obesity, compared to 37.9% of white and Asian adults, the report said.
Utah’s demographics — the population is more than 90% white, according to the Census Bureau — could account for part of its national ranking, but because the causes of obesity are disparate, there’s much more involved, including the predominant faith group in the state and its promotion of healthy lifestyles.
“We’ve seen that the large number of Mormons in the state have had an influence on behavior because of the religion’s belief about tobacco. I can’t speak to whether that also has contributed to combating or preventing obesity, but it’s worth investigating, because cultural differences impact behavior, too. That may be a factor,” Auerbach said.
Officials at the Utah Department of Health also hope that some new programs implemented over the past decade are already having an effect on Utah’s children. The State of Obesity report found that Utah, along with New Hampshire, had the lowest percentage of 10- to 17-year-olds with obesity in the nation.
Rebecca Fronberg, assistant program manager for Healthy Living Through Environment, Policy and Improved Clinical Care, said Utah has been the recipient of several federal grants dating to 2008, which has enabled it to establish programs promoting breastfeeding, which has been shown to contribute to healthy weights in children, and to teach obesity prevention in schools and child care centers.
The department has also expanded programs that promote wellness in schools, from eliminating sweetened beverages to incorporating physical activity throughout the school day, Fronberg said.
The role of sugary drinks in alarming rates of obesity has gotten widespread attention in recent years, with several cities, including Philadelphia, Seattle and San Francisco, enacting higher taxes on the beverages to try to reduce consumption. That’s one of the recommendations in the new report, along with expansion of other programs that could help people who are most at risk for obesity and related diseases.
A range of solutions
The report lays out a range of policies that the authors say could halt the spread of obesity and eventually reverse it. They include eliminating certain tax deductions for manufacturers who market unhealthy foods and drinks to children, provide more money for pedestrian and bike trails and safe passages to schools, prioritize physical activity in schools, and expand federal nutrition programs for mothers and children. For the latter, the authors recommend that the federal Women, Infants and Children (WIC) program cover children to age 6 and cover mothers up to two years after giving birth.
Auerbach said that states should be more aggressive about getting eligible women and children enrolled. “Nationwide, about 50% of eligible WIC have been enrolled. In Utah, for reasons I don’t understand, only 39% are enrolled. Part of our recommendation says that 50% is too low, so this is worth exploring,” he said, adding that full expansion of Medicaid would also help address obesity by making programs, such as one designed to combat diabetes, available to more people.
The report also urges expansion of Medicaid-covered services to include weight management programs and services for children.












