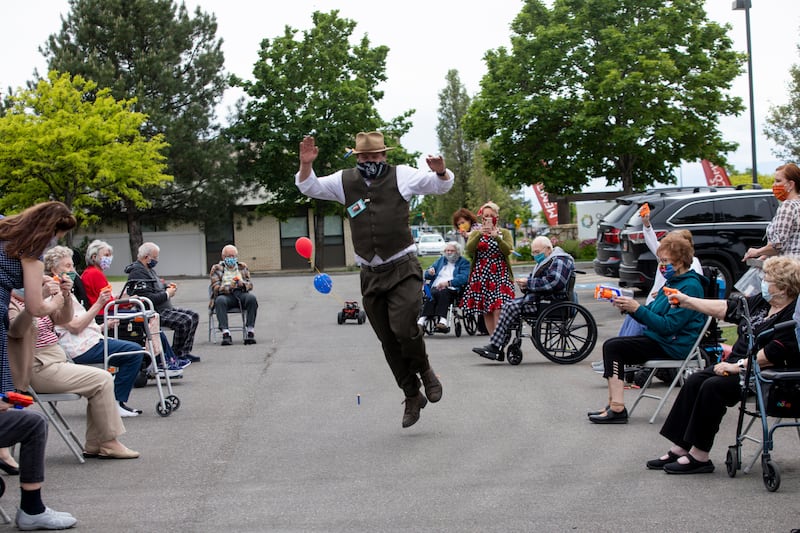SALT LAKE CITY — Not wanting to interrupt his brother’s birthday party, Mike kept ignoring his phone buzzing in his pocket. By the fifth call, he picked it up.
It was work. Could he please come in early?
By 11 p.m. on April 29, Mike was at the Salt Lake County nursing home where 21 residents had just tested positive for the coronavirus and needed to be quarantined — immediately.
Throughout the night, he and a fellow certified nursing assistant wheeled sleepy residents through the hallways into new rooms, separating them with plastic curtains. He apologized over and over again for the rush.
Mike, 25, asked to be identified only by his first name because he wasn’t authorized to speak about the facility. Normally as a long-term care rescue aide, he comes into facilities that need help and immediately learns his patients’ names, asks about their families. There was no time tonight. He promised to make it up to them somehow.
The stress was too much for his fellow aide, and the next evening Mike found himself the only nursing assistant in the quarantine unit, responsible for all 30 residents — still not knowing anyone.
Management reassured him at 6 p.m. that someone was coming, but two hours later broke the news that he was on his own.
They bought him a pizza instead.
By day 3 he had backup, but for weeks it was just the two of them — and besides normal patient care, which includes changing briefs, giving baths and delivering meals, they were also changing bed linens and mopping floors because no one from housekeeping wanted to risk getting infected.
“It is insane,” he says. “We get up and we run and we run and we run. We don’t stop. We don’t take breaks, we don’t get lunch. We pull 12 hour shifts — 12 on and 12 off, we just go, go, go, then the shift ends and we go and crash. Rinse and repeat. That’s just how it is. We just don’t have enough staff in order to do this.”
As COVID-19 continues its deadly march across the globe, nursing homes are taking the brunt of the impact.
Consider these sobering statistics:

- In the U.S., nearly 8 of 10 deaths from the coronavirus are adults over the age of 65. Fifty-nine percent are those over 75.
- Around 1.3 million Americans live in nursing homes and 800,000 live in assisted living facilities — together comprising roughly 0.6% of the population — yet deaths of residents and staff in those facilities make up between 35% to 42% of all U.S. coronavirus deaths.
- In Utah, 43% of the state’s coronavirus deaths have been in long-term care facilities, while Minnesota has one of the nation’s highest percentages with 81%. Rhode Island is at 61%.
Such outcomes are tragic, yet experts who study aging aren’t surprised.
The pandemic is just revealing to the public what they say they’ve known for decades: America’s long-term care system is broken, the consequence of having been ignored, overlooked and marginalized for years, endangering not just care recipients but those who care for them.
“It’s a crisis on top of a crisis,” says Barbara Bowers, a professor and associate dean for research at the University of Washington-Madison School of Nursing, and founding director of the School of Nursing’s Center for Aging Research and Education.
Yet while the pandemic will eventually subside, the graying of America will not — and by 2060, there will be 98 million seniors — double the number from 2015 — and 1 in 3 will need nursing home care at some point in their life.
Is this the best we can do?
“Care is the work that makes all other work happen, especially now,” says Stephen Campbell, data and policy analyst at PHI National, a nonprofit research and consulting firm that aims to improve the quality of direct care jobs. “Part of this is just about bringing care from behind closed doors and out into the public eye, no longer thinking of these (care) programs as ‘for them,’ but for all of us — that we all benefit from, and we should all care about.”

The need for care
Providing or arranging needed long-term care for a loved one is never easy — and it hasn’t stopped or slowed down just because there’s a pandemic raging.
Adam Benton, co-founder and senior vice president for Stellar Senior Living, which operates 12 senior and assisted living facilities across Utah, Colorado, Arizona, Idaho and Washington said people are still “voting with their feet,” and moving in, even if it means now only talking with loved ones through a window.
“It’s a little heartbreaking,” he says. “It just shows that people are there to support and love their parents, and also shows that they still think this is the best place for their mom or dad to be.”
Assisted living communities, which are state, not federally regulated, provide help with activities of daily living like personal grooming, cooking, housekeeping, maybe medication management, but don’t provide the full 24/7 medical attention and care someone in a nursing home might need. (See box for more definitions.)

Other families are waiting — hesitant to put their loved one into any type of group setting where they fear COVID risks might be greater, says Michelle Malais, owner of Assisted Living Locators of North Salt Lake.
She has several clients with dementia whose family has refused to move them anywhere, yet are absolutely exhausted by providing round-the-clock care at home.
“I don’t blame them,” she says. “It’s a scary situation.”
No matter where care is provided, family involvement is crucial, which is another reason the pandemic has been so hard.
Before COVID, family members frequently visited loved ones in Symphony South Shore to help with laundry, take them to church or just bring in a favorite cookie or soda, said TaNisha McSpadden, registered nurse and University of Chicago case manager for the rehabilitation and long-term care facility in Chicago.
Yet now, with families socially distanced to parking-lot parades or phone calls through closed windows — residents don’t get the same interaction, or Snickers bars, they were used to, she said.
Instead, McSpadden’s activity staff frequently takes around a juice or popcorn tray or the candy cart, “trying to keep them engaged in some type or normalcy,” she said.
The loss of family visits is not only distressing and isolating for residents, but adds work for caregivers, particularly certified nursing assistants — who are picking up the slack until families can safely return.
CNAs, or certified nursing assistants, perform most of the grunt work in nursing homes, daily tasks like helping residents use the toilet or changing their briefs, moving them from beds to chairs, getting them to meals or giving them baths, spending an average of 2.2 hours a day with patients —more than double the time spent by nurses.
Unlike registered nurses who have a degree, CNA is a entry-level, licensed position that is physically and emotionally demanding, leading to high turnover rates — often 100% — and employee burnout.
Because of that, nursing homes are chronically short-staffed, meaning it’s not uncommon for nursing assistants to have 10 or 12 patients daily, with as many as 20 or 30 at night.
COVID is making those ratios even worse.
Not only are families out of the picture, but if staffers get sick, or are afraid to come to work because they aren’t given personal protective equipment, it just means more work for those left in the facility.
Despite nursing homes being a highly-regulated industry, the federal government only mandates minimum staffing standards for nurses — not CNAs.
A nurse must be on duty for eight hours a day, seven days a week, but facilities only need “sufficient staff” to meet needs — a definition left to states’ and facilities’ discretion.
Advocates have requested a federal minimum staffing standard for years, says Bowers, but there’s always pushback from facilities, 69% of which are for-profit, because “it would be expensive to actually staff nursing homes at a decent level.”
It’s possible COVID could change that, highlighting that insufficient staffing can lead to decreased quality of care in the best of times — and tragedy during a pandemic, says Charlene Harrington, a professor emerita of sociology and nursing in the School of Nursing at the University of California, San Francisco.
When COVID hit, facilities with insufficient help, and who couldn’t compete with hospitals to get enough PPE, weren’t able to do the proper infection control measures and the virus spread, she said.
Yet outbreaks in nursing homes weren’t inevitable. Harrington believes if owners had invested in proper staffing and been able to get testing and necessary supplies, many deaths could have been avoided.
“I hope we’ve learned that we can’t have such short staffing in nursing homes around the country and expect to protect people,” she said.

A question of wages
Brittney Saez spent nine years working as a CNA in Utah County nursing homes, walking five or six miles during each nine-hour shift with few, if any, breaks.
She helped residents get up, get dressed, get meals, get medications, get showered, get into bed and out of bed, back and forth and back and forth — all for $12 an hour — and that was only thanks to nine years of experience.
The average pay for a CNA in Utah is $13 an hour, while nationally, CNAs average about $14.25.
Mike makes $16 an hour based on his experience, but he knows that’s above average. His wife, who’s been a CNA for nine years with different companies makes $11.25 — despite glowing recommendations from co-workers, Mike says.
Pay remains low because of how most nursing homes are funded.
Six out of 10 nursing home patients are covered by Medicaid — the government insurance for low-income adults and seniors, pregnant women, children, and people with disabilities — which also pays the lowest per-diem rate for long-term care, says Howard Degenholtz, associate professor of health policy and management in the University of Pittsburgh Graduate School of Public Health.
If the largest purchaser of care is paying the lowest price — you’ll get minimum quality and low staffing, he says. Unlike private-pay facilities, Medicaid-funded nursing homes can’t just raise rent in order to pay staff better — the government rate is fixed.
During this pandemic, 29 states have requested Medicaid waivers to temporarily increase their payment rates for Medicaid recipients, like nursing homes, to cover additional PPE, staff hazard pay and overtime.
Wyoming has given all of its long-term care facilities an additional $27.75 per patient per day — 15% of the daily reimbursement rate of $185.10.
The state expects to spend $1 million to $2 million extra for this pandemic boost, said Kim Deti, public information officer with the Wyoming Department of Health.
Facilities with COVID patients can also request additional funds — $206.35 per patient and $641.53 for those on a ventilator.
While encouraging, such solutions are only temporary.
Long-term change would require that states permanently increase Medicaid reimbursement rates, though the move is often unpopular, as it may require increasing taxes, says Degenholtz.
Utah requested no such emergency waiver, which means it’s unlikely Mike will see any sort of pay boost.
He was recently reassigned to another long-term care facility in Salt Lake County to open a COVID unit there. Although it’s close to home, he’ll keep living in a hotel to avoid infecting his wife, who’s also a CNA.
It’s tough, but this has only cemented his desire to become an RN and do this forever, despite the terrible pay.
“We risk life and limb every single day to help these people, hold their hands as they pass, make them as comfortable as possible,” Mike says, “and I know personally eight people on unemployment who are making more money than I am. You can make more money flipping a burger than you can make literally caring for people’s loved ones.”
Finding other options
So if nursing homes consistently struggle with staffing issues, low pay and appear to be a target during a pandemic, why are we still using them?
The bottom line is, COVID or not, Americans keep aging. They need care. And a nursing home may be the only option many can afford — because it’s the one Medicaid is most likely to pay for.
However, there are encouraging signs that’s changing.
In 1981, 99% of Medicaid’s long-term care spending paid for nursing home care.
By 2016, it had fallen to 43%, or roughly $55 billion — with the rest of Medicaid funds going instead to in-home care and support: aides who visit folks at home to help with bathing, dressing or meal preparation — a huge policy step forward, Degenholtz said.
It makes financial sense — the 2019 median cost for a private nursing home room was $102,200, while living at home and receiving six hours of care, five days a week was $35,880, according to Genworth’s Cost of Care Survey.
When people talk about nursing home alternatives, they often point to PACE, Programs of All-Inclusive Care for the Elderly, which use Medicaid dollars to keep older adults in their communities.
Instead of paying for nursing home room and board, the money funds a team of physical therapists, nurses, drivers, CNAs, recreation therapists, dietitians, primary care providers, etc., who visit older adults at home.
They also drive them several days a week to a local PACE center, where they interact with other participants, get a meal, visit the clinic, play games or do crafts.
Currently more than 51,000 older Americans are involved with 264 PACE centers in 31 states, says Robert Greenwood, senior vice president of public affairs for the National PACE Association. Ninety percent of participants are eligible for both Medicare and Medicaid, which means no out-of-pocket costs.
Participants don’t live together and with PACE centers currently closed, the risk of infection from COVID appears to be fairly low. Preliminary data show a 1.1% mortality rate from COVID among PACE participants, says Greenwood.
Degenholtz expects that the current pandemic will only accelerate the trend of in-home care, as families “think twice” about moving a loved one into a facility.
“To have home care and be able to live in their own home with dignity and autonomy,” he said. “I think that would be a very positive outcome after this crisis.”
Yet if living at home — even with support — isn’t possible, there are still other options.
Green House homes offer high-level care from round-the-clock medical and care staff, but in a small home setting — no more than 12 residents with private rooms/bathrooms — an ideal model for a pandemic, says Susan Ryan, a nurse of 40 years and senior director for The Green House Project.
The small-house model not only allows deep and meaningful relationships between staff and elders, but it’s easier to control infections, she says. To date, 245 of the 300 Green House homes across 32 states have reported and only nine of them have COVID cases — with only six deaths out of 2,653 residents, a 0.2% fatality rate. The Green House Project is also working with the University of North Carolina to formally collect and analyze data related to COVID.
On average, 42% of elders in Green House homes are on Medicaid and 85% have mild to severe cognitive impairment, like dementia, says Ryan.
In assisted living homes, older adults usually need more personal and less medical support, says Benton with Stellar Senior Living. Because of that, residents are often in better health when they arrive, which may be another protective factor in a pandemic.
Stellar has 1,000 staff members and 1,500 residents, with a total infection rate between 1% and 2%, Benton said. They’ve had zero cases in their four properties in Utah.
Many assisted living facilities don’t accept Medicaid — just private pay. This prices out many older adults, yet allows Benton the flexibility to provide hazard pay to compensate staff for the extra cleaning and pandemic-related care.
“The tricky part is, we’re still learning about COVID and there’s no guarantee that option A is safer than option B,” says Rodney Harrell, AARP vice president of family, home and community. “We do know that providing more options means that people have more choices and a better chance of picking the safest and best option for them.”
The trick is making the choices affordable for all older Americans — not just the wealthy.
Washington state is the first state to set up a public insurance fund to help pay for long-term caregiving. Their employee payroll tax of 58 cents for every $100 earned will start in 2022, with benefits accessible by 2025 — for a total lifetime benefit of $36,500.
It may not sound like much, but the state calculated it would provide up to 5 years of respite care, or one year of part-time in-home care, or eight to 12 months of assisted living care, or four to six months in a nursing home.
“For 40 years, we’ve known that we had a model of care that needed to evolve,” says Sheryl Zimmerman, distinguished professor and co-director of the Program on Aging, Disability, and Long-Term Care at the University of North Carolina at Chapel Hill. “We have been evolving, but what we’ve got now is a big huge shove to be doing it even better.”