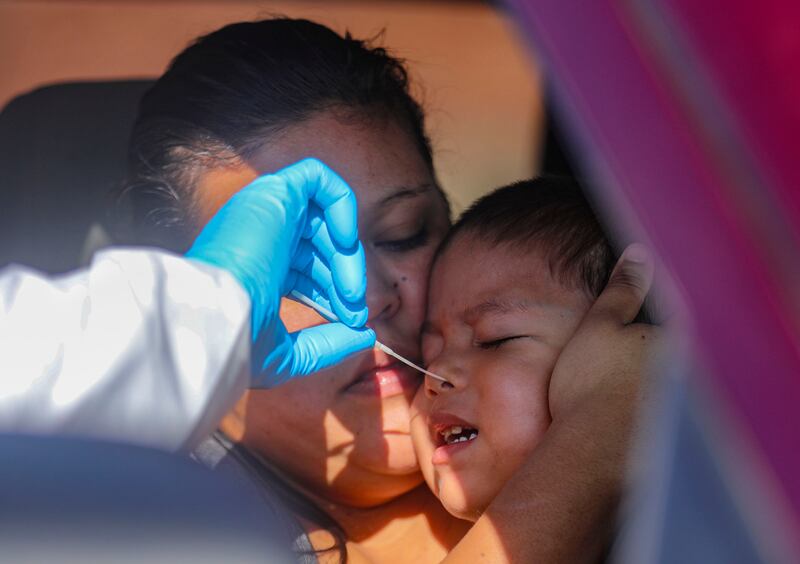
MONUMENT VALLEY, San Juan County — Kyler Wagner wriggled in his mom’s lap as what looked like an astronaut leaned through the passenger window of his grandfather’s truck and told him softly that he needed to be still while she inserted the longest Q-tip he’d ever seen into his nose.
His mother, Tyana Phillips, tightened her embrace and leaned her face against the crying child’s head, as the woman — dressed head to toe in white and wearing a plastic shield over her masked face — leaned through the window to administer the COVID-19 test in the parking lot of the Utah Navajo Health System’s Monument Valley Clinic, just a few miles from where she lives with her parents.

“We came just to be on the safe side,” said Phillips, 21, who decided to get tested with her son and father after her mother, who is on dialysis, was tested at the free mobile testing event on April 17. “We don’t have symptoms, and we’ve been trying to stay home and be safe. But I just wanted to be sure.”
Phillips was like a lot of people who showed up to be tested at the first of three mobile testing events that were a unique collaboration between the Utah Department of Health’s Public Health Laboratory and the Utah Navajo Health System. While most testing requires symptoms, a screening or a referral from a health care provider, these three events over the last six weeks offered testing to anyone who wanted it — without condition — even to residents of other states.

“Mass, open testing remains crucial to our goal of isolating infected people,” said Byron Clarke, CEO of the Utah Navajo Health System. “It really is the best tool for getting the bigger public health picture of all our other treatment efforts and tells us where we can improve.”
Whether it’s business owners hoping to reopen or public officials looking for data on which to base decisions, if there is one thing most people agree on, it’s the critical importance of testing. The results of that testing was part of the rationale used by Bluff Mayor Ann K. Leppanen and the Bluff Town Council to request to remain at red or high-risk level in an area of the state that’s been hit the hardest by the pandemic.
The state denied that request Wednesday and the town will be in an orange or moderate-risk level.
Some debate the value of asymptomatic testing, with cost being the main deterrent. But for Utah officials responding to the outbreak on the Navajo Nation and surrounding San Juan County cities, it’s been an investment that’s provided a more accurate picture of the problem. And that’s a rare advantage with a new virus and so many unknowns.
“Symptoms-only testing is fairly easy to do,” he said. “You just need tests, and those are becoming more available. Open criteria testing is hard to do (because) it takes tons of resources. Each two-day testing event takes about 1,400 Utah Navajo Health System employee hours to complete and costs about $30,000 just in wages, let alone opportunity costs. But it is the best way to get ahead of the spread and identify people who need to isolate.”
The information provided by the three testing events hasn’t just been helpful to those caring for tribal members.
“It’s definitely helpful to me,” San Juan County Health Director Kirk Benge said. “Up until this time (Monday night), I had only seen about 150 tests performed in Blanding, and less than 30 tests performed in Monticello. So I felt like it was a little bit of a black hole, compared to the data I had in Montezuma Creek and Monument Valley.”
While Benge learned there were more positive results than he expected, the number of cases caused by community spread (no known exposure) was minute. While Benge officially oversees the entire county, his department relies on Utah Navajo Health System to investigate and track cases within the reservation’s boundaries. Their cooperative effort is critical to understanding and containing the outbreak within reservation boundaries.
The Navajo Nation has an impressive record on testing, administering 27,162 tests through Wednesday. That’s about 13% of the Navajo Nation residents who’ve been tested.
Sadly, 146 tribal members have died from COVID-19 and 4,253 have tested positive.
Clarke said 17% of the those tests were administered to tribal members through Utah Navajo Health System’s collaboration with the state’s mobile testing crew. In the Utah section of the reservation, where about 8,000 tribal members reside, only 149 of the 4,356 tests tracked by Utah Navajo Health System were administered by other health care providers like Indian Health Services or private health care providers to tribal members.

Utah Navajo Health System is tracking 309 positive COVID-19 cases, with 288 of those tested by the one of health system’s clinics or the mobile efforts. Results from the mobile testing done in conjunction with the health system isn’t yet available as a separate category of testing and results, although state officials expect to have that in the next few days.
‘It just runs rampant’
Despite the cost of unfettered testing, Clarke said the value of the information gained, especially to individuals, is worth every minute and every penny.
“The majority of people who turn up positive had no idea they were even sick, so without test results, they could not have known that they needed to be extra careful for a few weeks until they recovered,” he said.
Kelly Carnahan, emergency response manager for the state’s public health laboratory, has spent every day since they created the mobile response unit on the road testing in places like jails, elderly care centers, homeless shelters, rural communities and Native American reservations. She said they’ve traveled to one long-term care center five times to do testing that wouldn’t be possible otherwise.
“What’s happening is asymptomatic health care workers are bringing it into the facility and not even knowing they’re carrying it,” said Carnahan as she drove to a testing site in Delta before the sunrise. “They bring it in without knowing it, and the people who are residents, they are contracting it and becoming very, very ill.
“And nobody can figure out where it’s coming from because they’ve been locked down, not allowing visitors or family members. And it just runs rampant.”
In fact, 41 of Utah’s 92 COVID-19 deaths are residents of long-term care facilities, as of Thursday. Maybe more important, viral outbreaks have impacted 112 facilities with 217 residents testing positive and 196 of health care workers in those facilities testing positive.
Carnahan hopes the mobile unit’s testing gives public health official and elected leaders better information to make decisions about a constantly evolving virus.
“I hope it gives them some clarity on how to manage,” she said. “We’re finding people who are still positive three weeks later. They were tested at one event, and then they come back and they’re still positive, but they don’t feel sick. There is confusion. Hopefully it just gives them much better information on how to manage all of their infectious disease protocols.”









Multiple borders
The Navajo Nation sits on the corner of three states, and while it makes for a rich and interesting community, it also leads to myriad jurisdictional issues that can be contentious and difficult to navigate. In the case of COVID-19, public officials worried jurisdictional issues could be dangerous, even deadly.
“One of the most frustrating things in this part of the state is that the community overlaps borders,” said Benge.
“People shop in Colorado and New Mexico as much as we shop in Blanding, oftentimes. So I think one of the desires that Utah Navajo Health Systems has had, and we’ve had as a public health department, is to try and treat the community as a community and do what’s best for the community and not let ourselves get overly focused on dividing things up on tribal lands or state lines. UNHS has been very devoted to that.”
Clarke said they believe that once officials put restrictions on who can get tested, in any way, they lose valuable data.
Of the 4,356 tests administered by Navajo Health System, 1,228 tests were given to residents of Arizona (1,129), New Mexico (52), and Colorado (47). The health system has about a 7% positive rate, which is higher than Utah’s rate of around 4.3% positive.
While Summit County has earned a lot of attention for dealing with one of the state’s first and most extensive outbreaks, San Juan County actually has a higher infection rate. San Juan County’s infection rate is 1,624 per 100,000 residents with a total of 251 cases, while Summit County has an infection rate of 963 per 100,000 residents with 404 cases.
“This testing is highly important,” said Shawn Begay, public health director for Utah Navajo Health System. “It lets us know where we stand as a nation, like what trends are going on? Are we rising? Are we stabilizing? Or are we going back down?”
Of San Juan County’s 251 positive tests, 239 of those are considered Utah Navajo Health System cases, which means they’re most likely on the reservation, although they do provide health care services to many nonnative residents of the county, as well.
Of the state’s total cases 286 (3.6%) are listed as American Indian or Alaska Native, even though they are just 2.3% of Utah’s population. They have the third-highest case rate, behind Hispanic/Latino (37.8%) and white (39%), but the second-highest hospitalization rate, trailing only Native Hawaiian/Pacific Islander.
The mobile unit held free testing events at all four Utah Navajo Health System clinics, starting with Navajo Mountain, which had two high-profile deaths within the first week of the Navajo Nation outbreak, followed by two days in Monument Valley, two days in Montezuma Creek and two day in Blanding, which is not on the reservation.
Cooperation between government and health care providers has been critical, especially when it comes to dealing with a hot spot. Benge said without Utah Navajo Health System, he’s not sure how he would accurately investigate the cases of people in his county who reside on the reservation.
“I don’t even know how I would speculate what it would be like,” he said. “My board of health would really like San Juan to treat our entire county as a community, and not let ourselves get bogged down in jurisdiction. ... We’re committed to protecting all county residents, regardless of jurisdiction.”
That is made possible because Utah Navajo Health Systems can do the kinds of investigation necessary to confirm where someone lives, as well as complete the critical contact tracing necessary with a highly contagious virus like the coronavirus.
“Their efforts have been invaluable in understanding the impact of this on our community,” Benge said.
He said that if Utah Navajo Health hadn’t “gone and done this push on the reservation” there might be more spread in the county. That’s because while officials knew there was an outbreak on the reservation, they weren’t sure how extensive it was in Utah and they weren’t sure how many of those positive cases were without symptoms.
“What we’ve learned is testing for symptomatic persons has been helpful,” he said. “I worried we might have a lot of undetected cases, asymptomatic cases, especially in Blanding. ... It helped us understand what is really going on, and that’s been very valuable.”
‘Crazy new world’
Both public health and medical officials said the testing has confirmed the wisdom of the advice being offered since the outbreak began.
“What we learned is ... don’t let down your guard,” said Dr. Bill Cuskelly, a 30-year veteran of medicine who has worked at Utah Navajo Health System for the last five years.
“(COVID-19) is real, it’s out there, and there are a lot of people who have minimal symptoms, so being very cautious by maintaining social distance, wearing masks in public and hand-washing, we can reduce the spread. It reinforces those recommendations. It’s real easy for us to be complacent over time, especially as we get used to this new normal. And we need to guard against complacency.”
Benge is making decisions about when and how businesses reopen, while Clarke and his staff are offering advice to residents of the Navajo Nation, who are living under much different circumstances than their friends and families living off the reservation. On the reservation there are nightly curfews and weekend lockdowns, while off the reservation, San Juan County is listed as yellow, with the exception of Bluff, which is listed as orange.
Complicating every decision-making process is the uncertainty surrounding COVID-19. Because it is caused by a new coronavirus, information is changing, advice is evolving, and many people are expressing frustration with the lack of absolutes.
Carnahan acknowledges that uncertainty and hopes people understand that as researchers acquire more information, the guidelines, including symptoms and advice, may shift. But she feels certain about one thing.
“I really don’t think there is a disadvantage to (mass) testing,” she said. “The more people we can provide testing to, the more we understand, and what we’re truly finding is those asymptomatic carriers. That allows us to start to understand where the virus is spreading.”
And while there are “at-risk” populations, she cautions anyone from feeling overly confident about the virus.
“I have learned this virus doesn’t really care who ... it targets,” Carnahan said. “You have elderly people who are asymptomatic and young people who get very sick. ... Every single thing we’re doing in this pandemic is new. ... We’re learning as we go; there are going to be glitches. But we are addressing those issues, as they happen. ... It’s just a crazy new world.”
Whatever the future holds, most involved in the mobile testing efforts acknowledge Utahns are lucky to have what Carnahan calls “a unique animal.” She’s helping to train National Guard members so they can expand mobile testing opportunities.
“I don’t think there is a disadvantage to (investing) in mobile testing,” she said. “The more people we can provide testing for, the more clarity we have, and what we’re truly finding is those asymptomatic carriers, and we’re really starting to understand how the virus is spreading.”
In her mobile testing efforts, she hasn’t seen the numbers anywhere else that she’s seen on the Navajo Nation.
And that’s created an almost paralyzing fear for some living on or near the reservation. Phillips said what motivated her to get tested was peace of mind. Carnahan said that across the state, since the beginning of the outbreak, that is a common theme, especially if they are or if they live with someone considered high risk, like Phillips does.
“I don’t know how many phone calls I took from people saying, I can’t go to IHC or U. of U., or being confused about whether or not testing was free,” she said. “People are scared. They just wanted to be tested, even just for peace of my mind.”