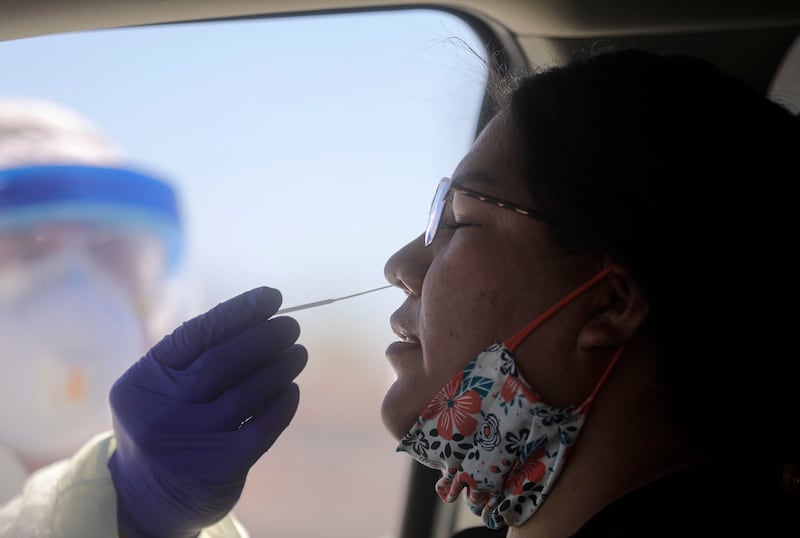
MONTEZUMA CREEK, San Juan County — Shawna Whitehorse didn’t drive to a mobile COVID-19 testing site because she was sick.
She hopped in a car two weeks ago with several other health care workers from the Utah Navajo Health Systems and drove 66 miles because a supervisor encouraged them to do so.
“I went down to Monument Valley and got tested, and then, I guess that Sunday, three days later, I got a call from public health saying that I was positive,” said Whitehorse, who works as a fleet manager and an advanced EMT for Utah Navajo Health Systems. She was the only one in the group who tested positive. “It was just kind of a shock because I was like, ‘I don’t really have symptoms.’”
And as a health care worker, she’d paid attention to the most common symptoms — cough, shortness of breath and fever.
“The symptoms I’d been having were more like back pain, body aches, and sometimes I would notice the joints of my hands would kind of hurt,” she said. “I already have sinus issues ... so I already have diminished sense of smell, so I didn’t think that was a real big issue. I really didn’t notice that I did lose my sense of smell and sense of taste.”
In fact, she didn’t realize that it was due to COVID-19 until she could smell and taste things like she normally had a few days ago.
Whitehorse is one of an estimated 9,000 health care workers in the U.S. who have become sick with COVID-19, even as they try to keep patients safe. Like her colleagues, she took every precaution recommended, and yet, she still got sick.
After the shock, she fought fear.
She is married with a 5-year-old son, and he has asthma and tonsillitis severe enough that she and her husband have made trips to the emergency room with him.
“So with this COVID being a respiratory issue, it was kind of scary,” she said. “I really didn’t want my son to get it, but then, at the same time, I’m working in EMS (emergency medical services).”
And knowing the precautions she’d taken to protect herself and the patients she treated, she began to understand just how contagious the new coronavirus really is.
“The thing about it, I wasn’t really anywhere,” she said. “I was mainly at home, and the demands of the job I was working, we had to do clearance before we could even go in the building.”
Utah reported 142 new confirmed COVID-19 cases on Monday for a total of 5,317. There were five new hospitalizations, with a total of 436, but no new deaths reported since Sunday. In Utah, 50 people have lost their lives to the illness caused by the new coronavirus.

Dr. Angela Dunn, state epidemiologist said the state still has a 4.2% positive rate, even as Utah continues to be in “a plateau.”
“One of the important things we track is where positive cases were likely exposed to the virus,” Dunn said. Community spread — or those cases caused by unknown exposure — is dropping.
“Only 11% are considered to be community spread,” she said, adding that “60% were exposed by someone in their household, 25% were exposed by someone they know outside their household.”
She said 4% of cases were exposure at work.
The state has now administered 124,661 tests — up more than 2,000 overnight.
Dunn also said the state is actively monitoring the outbreak in San Juan County, as half of the cases now reported in the rural area were confirmed through testing in just the last week.
Whitehorse’s case, confirmed through the state’s first mobile testing effort in Monument Valley, is one of 94 reported by Utah Navajo Health Systems, and one of 116 cases in San Juan County. She, her husband and son took advantage of free mobile testing by the Utah State Health Department’s Public Health Laboratory on Friday in Montezuma Creek at the clinic where she works, despite the fact that none of them have symptoms right now.
The number of cases in a county of about 17,000 may seem alarming. But Kirk Benge, San Juan County’s public health director, said it just confirms what officials suspected because of the outbreak on the Navajo Nation.
“I view it as an existing outbreak that we’re uncovering through testing,” he said. “I think the testing is just catching up to that. ... We know there is an outbreak on the reservation. but our positivity (rate) hasn’t been surprising to me.”
Dunn said the number of positives is something state officials are monitoring to make sure officials “have the capacity they need to control it.”
“(Testing) tells us who is actively infected,” she said. “It is a true spike in cases. It’s true they had limited testing, and there were likely cases we missed in weeks prior, but the spike is real. It’s active cases.”
Benge said he felt like the tests confirmed what they knew to be the case, and at a rate that the county’s hospital systems can manage. He feels like having data to back up the request by health department officials to use mitigation efforts like washing hands and social distancing helps persuade the public that the virus is indeed in San Juan County, and precautions should be observed.
He said drive-thru testing will be offered in Blanding, and he hopes anyone who believes they’ve been exposed or anyone with symptoms would take advantage of that drive-thru service.
A few hours after Dunn’s press call, the health department was able to release all the test results for last week’s mobile testing event — which spanned three days and two locations in San Juan County. They administered 1,477 tests with 88 of those confirmed for COVID-19. That is a positive rate of 5.9%. Not all of those 88 positives were included in San Juan’s 116 reported cases as of midday Monday. They will be in Tuesday’s results.
The mobile lab also tested residents of the Navajo Nation who live in Colorado, New Mexico and Arizona. Only Arizona had positive cases with 58 positives out of 940 total tests, according to data from the Utah Navajo Health Systems.
The largest jumps were San Juan and the Wasatch Front, with 49 new cases in Utah County and 62 new cases in Salt Lake County.
In Utah County a ‘strike team’ was dispatched last week to help contain an outbreak at a residential facility for adults with disabilities.
“(The response) is tailored to the needs of a situation,” Dunn said, adding they can supply health care professionals personal protective equipment and training on how to use it, as well as investigators to identify exposures and testing.
The response came after 15 of the 40 residents tested positive and nine of the staff was confirmed to have COVID-19. The residential living facility doesn’t have skilled nursing on staff and didn’t have medical supplies to limit the spread of the virus.
A breakdown of Utah COVID-19 cases, hospitalizations and deaths by health district:
- Salt Lake County, 2,769; 251 hospitalized; 31 deaths
- Utah County, 1,122; 61 hospitalized; 9 deaths
- Summit County, 377; 33 hospitalized; 0 deaths
- Davis County, 299; 24 hospitalized; 2 deaths
- Weber-Morgan, 167; 21 hospitalized; 2 deaths
- Wasatch County, 165; 7 hospitalized; 1 death
- Southwest Utah, 119; 13 hospitalized; 2 deaths
- Bear River, 62; 10 hospitalized; 1 death
- Tooele County, 71; 6 hospitalized; 0 deaths
- San Juan County, 116; 12 hospitalized; 2 deaths
- Central Utah, 25; 2 hospitalized; 0 deaths
- Southeast Utah, 11; 0 hospitalized; 0 deaths
- TriCounty (Uinta Basin), 14; 1 hospitalized; 0 deaths