The number of monkeypox cases in Utah continues to climb, but it’s not clear how many cases there have been so far.
The Centers for Disease Control and Prevention is reporting 13 monkeypox cases in Utah. But the Utah Department of Health and Human Services has recorded only 11 cases in the state — eight in Salt Lake County and one each in Utah and Davis counties, and the area served by the Weber-Morgan Health Department.
Utah state epidemiologist Dr. Leisha Nolen said a similar difference in the count recently was due to a Utah resident being diagnosed with the virus in California, and California authorities alerting the CDC but not passing along the information to Utah.
“That’s where the errors come in,” Nolen said. “We would like to have those updates, certainly if the person comes back to our state so we can make sure to connect with them, make sure they’re able to isolate and prevent the spread to other people, as well as find out if other people have been exposed.”
Monkeypox, usually confined to parts of Africa, has spread globally, mainly in men who have sex with men. As of Monday, the CDC said there are 1,972 cases in the U.S. The virus started showing up in the United States in early May and later that month, two Salt Lake County residents were identified as Utah’s first cases.
Nolen said all of Utah’s cases are in men, and those most at risk are likely to have had around 10 sexual partners within a few weeks. She said the state looked at rates of HIV and sexually transmitted diseases to determine the distribution of Utah’s federal allocation of the smallpox vaccine approved for use against monkeypox.
“Right now, the outbreak throughout the country, throughout the state, throughout the world is really within a specific population,” the epidemiologist said. Because intimate contact is usually needed to transmit the virus, she said “for the general population, who aren’t having these kinds of relationships, I think it’s not a high risk.”
Still, Nolen said, monkeypox “certainly is an infection that could go to other people. It’s just taking advantage of social networks. So we are concerned that the infection could start spreading through different social networks that would involve skin contact. So it’s something I think we need to watch and we’re trying to get under control.”
While the virus can be transmitted through nonsexual contact and even bedding or other materials used by an infected person, Nolen said she’s aware of only a couple of cases, in Canada, where someone became infected without direct, skin-to-skin contact.
Utah has received two rounds of the vaccine, a total of 1,470 doses, and expects another 819 doses ordered last Friday to arrive shortly, she said. Within the population defined as high risk, Nolen said even those vaccinated before the U.S. ended routine smallpox vaccinations in 1972 should get the shot.
The Salt Lake County Health Department is already out of the vaccine.
“We had a private vaccine clinic on Thursday for people at the highest risk of transmission (determined by the Utah Department of Health and Human Services to be men who have sex with men and have had multiple partners in recent weeks) and gave 525 doses,” Salt Lake County Health Department spokesman Nicholas Rupp said.
Rupp said the shots will be offered to additional specific, high-risk populations that have yet to be identified when more doses are available. The vaccine is not available from other providers and it is not known when the federal government will allocate more doses to Utah, according to the county health department’s website.
None of the Salt Lake cases have been identified as picking up the infection in the county, Rupp said.
“Given that we have identified no local transmission, and that monkeypox transmission requires significant, close contact, Sat Lake County residents in general do not need to be concerned at this time,” he said. “People with multiple intimate partners, particularly men who have sex with men, should be aware and avoid sexual or intimate contact with people with symptoms.”
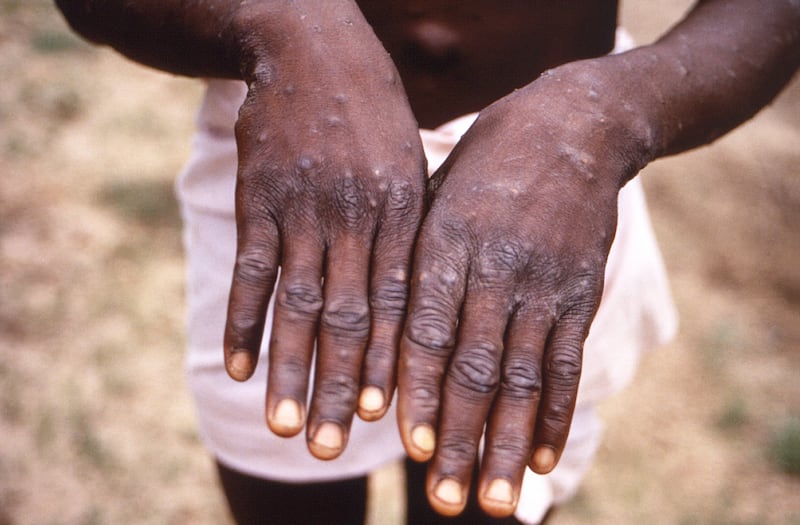
Early symptoms include a fever, headache, muscle aches, backache, swollen lymph nodes, chills and exhaustion, then within a few days, a rash develops, often starting on the face or in the mouth before spreading and developing into fluid-filled lesions that eventually scab over and fall off.
Nolen said there have been “a few cases” where men have become infected with monkeypox from contact with someone in Utah but “all the people we’ve had have been very cooperative about who they’ve had contact with and we’ve been able to follow up with those people.”