More people think the COVID-19 pandemic’s ongoing than don’t, according to a new HarrisX poll for the Deseret News. That’s despite the fact that the U.S. Department of Health and Human Services declared the public health emergency in America over nearly a year ago, on May 11, 2023.
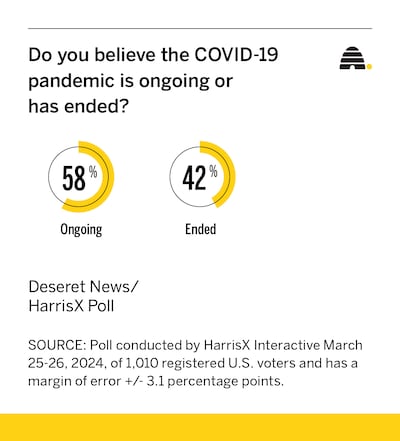
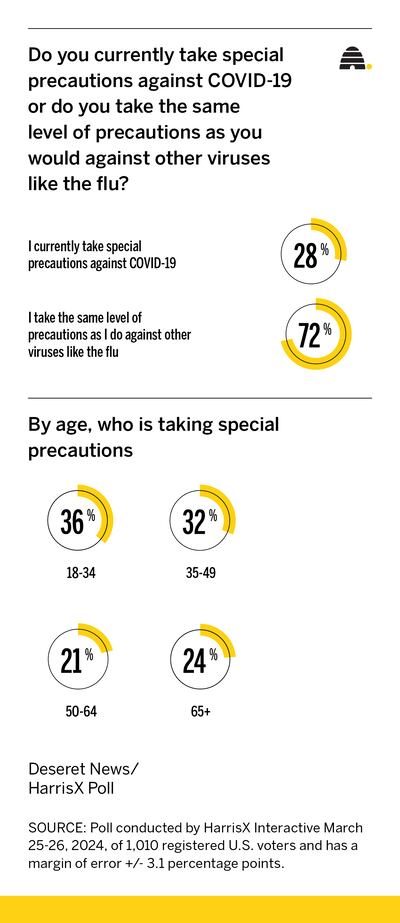
The poll, conducted March 25-26 by HarrisX of 1,010 U.S. registered voters, found 58% believe the pandemic is ongoing, though few are still taking precautions (28%). Seventy-two percent said they take the same precautions they take for the flu. The survey has an error margin of +/- 3.1 percentage points.
Han Kim, a professor of public health at Westminster College in Salt Lake City, thinks lots of people don’t understand the difference between a pandemic, an epidemic and an illness that — however dramatic it was in the past — has settled into an endemic phase, meaning it’s established and circulates, but not at its former scary level.
“In the first few years, the virus had a huge advantage in that none of our immune systems knew what to do with it, but now it’s been out a while and because so many people have the vaccines or had COVID, it seems like our immunity is kind of coming into balance with the virus.” Kim said.
While it’s well established that COVID-19 takes an especially harsh physical toll on older people, the survey found the group most likely to be taking precautions is those ages 18-34 (36%). Just under a quarter of those 65 and older are being extra careful, compared to those 35-49 (32%) and those 50-64 (21%).
Kim suspects that could align with political views: Young people tend to be more liberal, older more conservative. And studies and surveys, including this one, repeatedly show that Democrats (41% in this poll) take more special precautions against COVID-19 than Republicans (19%).
COVID-19 is no distant memory; the impact remains vivid in many minds. More than half of those surveyed (53%) said COVID-19 closures and restrictions affected their mental health at least somewhat negatively, compared to 31% who said it didn’t impact their mental health. Among women polled, 57% report a negative impact on mental health, compared to 49% of men. Just 12% and 20%, respectively, said the mental health impact was somewhat positive.
Han sympathizes. “In terms of disease dynamics and popular sentiment, COVID is still a new thing and it’s still a trauma that’s really quite fresh in most of our minds.”
‘It hasn’t ended’
Those polled were nearly evenly divided on whether they’d tested positive for COVID-19 at some point. And 3 in 10 reported experiencing the lingering version that’s been dubbed long COVID-19, with various persistent symptoms.
The poll found partisan differences in the view of COVID-19 as an ongoing problem, with 68% of Democrats saying COVID is still a problem, compared to 49% of Republicans. Women are more likely than men to say the pandemic is ongoing, 62% vs. 55%. And while majorities of all age groups say the pandemic is not over, that’s especially true of older people. Two-thirds of them say it is ongoing, which drops to about half among the youngest group, 18-34.
Broken down by race, the survey found a far larger share of Black people (71%) and Hispanics (69%) believe the pandemic is ongoing, compared to white people, at 54%. That’s true, as well, of liberals (69%) and moderates (64%) compared to conservatives (46%). College grads were somewhat more apt to know the pandemic is officially over compared to those with less than a four-year degree, 56% vs. 60%. Differences by income are clear as well, with 61% of those earning below $75,000 a year saying the pandemic is ongoing, compared to those who are wealthier (53%).
Dr. Eric Natkin’s patients are figuring out the right balance of careful and more carefree. At R2 Medical Clinic in Denver, he said, “Many individuals express a heightened sense of awareness and concern regarding their overall well-being, with an increased interest in boosting their immune system and maintaining a healthy lifestyle. Conversations often revolve around the safety and efficacy of the COVID-19 vaccine, with people eager to understand how their existing health conditions and the treatments they are undergoing might interact with the vaccine.”
It calls for clear, evidence-based communication tailored to the patient, he said.
He also noted that as people seek wellness therapies as part of preventive health, they talk about mask-wearing and social distancing in the context of being treated. “While the majority adhere to recommended safety protocols, there’s a noticeable variance in comfort levels, reflecting the broader societal debate.” The interactions are diverse and prove “personal experiences, health priorities and the changing nature of the COVID-19 pandemic deeply influence individuals’ perceptions and actions toward health and safety measures.”
No longer pandemic, but possibly risky
Dr. Leisha Nolen, state epidemiologist in the Utah Department of Health and Human Services, said that while the pandemic officially ended nearly a year ago, COVID-19 still makes people sick and kills some. But public health officials now liken it to a seasonal endemic, which means it’s around, but more akin to the flu. Vaccines, people getting COVID-19 and developing natural immunity, and other factors — including mutations to milder strains and development of helpful antiviral medication — have led to that.
That could change, Nolen said. But COVID-19′s not nearly as frightening as it was in the early days. “I think the most important thing for people to know is COVID-19 is still there but we expect this to be something that’s going to be around for the long term,” like other seasonal ills. They still pose risk and some people do die, but “happily, it is getting to be less of a threat to people to be significantly severe.”
Dr. Paul Offit, a pediatrician who directs the Vaccine Education Center at Children’s Hospital of Philadelphia and a voting member of the FDA Vaccine Advisory Committee, points out that COVID-19 was not eradicated and still causes 1,000 to 1,500 deaths a week. Flu and RSV both kill still, too, but people have learned to do their best to protect themselves and live with them. “I think this will join those viruses,” he said.
Nolen said it’s appropriate for those who have weakened immune systems or their families to be concerned. “I think it’s difficult for those people to figure out what’s the right balance of being protective vs. getting back to their life.”
But she was surprised when the Deseret News told her that those most apt to be anxious and taking precautions, according to the poll, were young adults.
Kim was surprised, too, but could think of several things that might explain it, noting that as a college professor he interacts with many young adults and they discuss these things. He thinks they might be worried about long COVID and how it could impact their futures. Some could be protective of more vulnerable loved ones, like parents and grandparents. He also thinks it’s possible that young people worry because they are the ones who had their lives most disrupted by pandemic shutdowns. They were isolated from peers during a period important to social-emotional development. More of them lost jobs, had to do school online, were cut off from friends, missed graduations and other milestones, and both academically and socially fell behind.
Kim noted many have not caught back up.
When people are scared or anxious, experts said, it’s likely they see themselves in a high-risk group.
Those most vulnerable include people who are older — mid-70s now and older are believed most vulnerable by age — and people with chronic disease who might get sicker than most, those with weak immune systems and pregnant women. Combined, they make up the four big risk groups and the people that most countries are now targeting with vaccine campaigns, Offit said. “I think those people are appropriately worried enough to have a booster every year; it makes sense.”
The fear about long COVID, which spans age and other demographics, is that “this is going to be a long-term, debilitating infection for them,” he said.
According to Offit, research is pretty clear that three doses of vaccine lessens risk of COVID-19; but after three, there’s less evidence of efficacy. His advice to those at greater risk is to test themselves if they feel sick and if it’s COVID-19, make sure a doctor prescribes an antiviral immediately. “Don’t let your doctor tell you let’s wait a few days and see whether or not this gets better. That’s bad advice.”
Finding balance post-pandemic
Nolen said she really hopes that “people go out and live their regular lives and don’t have high stress about this. But I hope they still listen so that when we say it’s time for a new vaccine, they’ll see their doctor and get that vaccine. Or if we say that there is a scary new variant, they’ll know to protect themselves. I really hope that doesn’t happen. But we just want people to go about their lives but not completely forget to keep an eye on what’s happening,” she said.
That’s what Janice Lim, 28, of Palo Alto, California, is doing. An avid outdoor travel writer, she told the Deseret News she’s no longer worried, though she’s taken some precautions: She is fully vaccinated, “as it gives me peace of mind wherever I’m traveling in the future.” She takes hand sanitizer along when she camps. But, she adds, “I prefer to be able to breathe in the fresh air rather than wearing a mask even if the places I’m in are more crowded. It also doesn’t feel good to perspire in a mask.”
Her age and good health make her comfortable with her choices, she said. “I worry more about mountain lion attacks than falling sick at this stage of life.”

Kim stresses that public health is about balance and COVID-19 revealed a lot of trade-offs. “We need to find a balance between trying to prevent spread as much as we can but realizing we can’t prevent all spread without shutting everything down again. And that has long-term consequences as well, including mental health. ... We’re going to see those effects play out for the next probably several decades, how that’s impacted people’s wellness and health.”
Many haven’t recovered economically, he said, which plays a big role in health. He suspects there’s increased anger and anxiety related to both the disease and how it was managed, including the fact that measures that kept people somewhat physically safe led to job changes and challenges like paying rent and social isolation.
There’s no “pat answer,” he added, to how to balance the harms of the virus itself against the harms that accompanied it.



