In 2025, the United States had its worst measles outbreak in decades, including the first children to die from measles in 20 years. It’s 2026, and measles cases seem to only be getting worse: 2026 cases have already reached 50% of 2025’s total cases in just two months. Utah has been a hotbed for measles cases, accounting for nearly 1 in 3 of all cases in the United States, with most cases occurring in the southwestern counties.
The recent outbreak is likely a direct result of declining measles immunization rates. Improving immunization rates against measles will be vital to reversing its spread in our community. Recent models suggest that if measles immunization rates decrease just 10%, the United States will see an estimated 11 million cases of measles over the next 25 years (an average of 440,000 cases per year). In contrast, if we can increase immunization rates by 5%, there will be only 5,800 cases over that same time frame (an average of around 200 cases per year).
Measles is far more than a rash and fever — it is pneumonia in a previously healthy child, brain swelling in an intensive care unit and anxiety for families who thought it was gone. At its core, measles prevention is about protecting children, especially those who are too young or too medically vulnerable to be fully protected themselves.
As a hospital-based pediatrician in Utah, I want to help keep children safe, healthy and out of the hospital. Below are 10 important questions Utah parents should get answered about measles recognition and prevention.
Is measles really that dangerous for children?
Yes. Measles can be very dangerous and even life threatening, especially in infants. It is extremely contagious, and many children with measles are hospitalized due to complications. Of those, 1 in 1,000 dies.
What are the first signs and symptoms of measles?
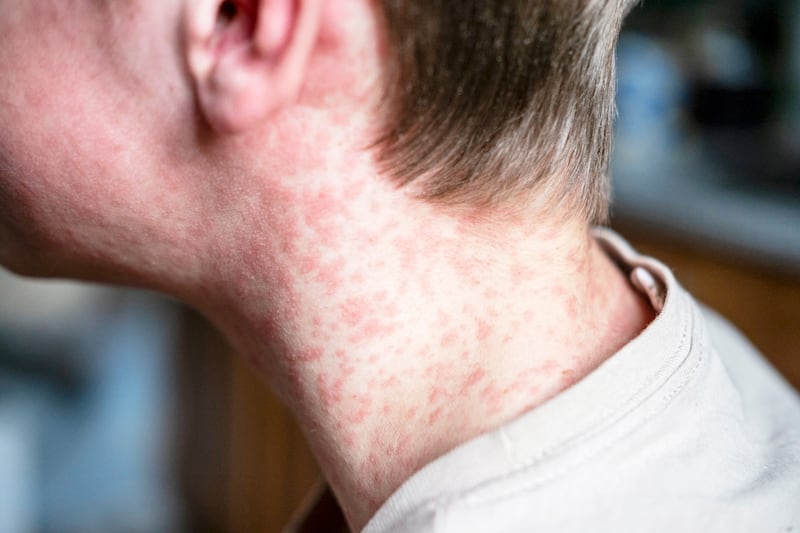
The first signs of measles include a fever, runny nose, cough and red eyes. A few days later, a red rash can appear that starts on the head and spreads downward.
My child was exposed; when might I see symptoms?
Measles symptoms usually take one to two weeks to start after exposure (longer than most viruses). If your child is immunized, the chances of them getting measles are very low.
How contagious is the measles virus?
Measles is extremely contagious; it can spread through the air and survive for two hours in a room after a person with measles has left it. A person with measles will spread it to 90% of unimmunized people they have contact with. Those with measles should quarantine until at least four days after the appearance of their rash.
I think my child has measles, what should I do?
If you suspect your child has measles — especially if they have been exposed recently — you should call your health care provider for guidance. They will help you know where to get tested. This will help you know what to watch for and avoid spreading it to others.
Please call the facility before you go to notify them that you plan to come for testing, and wear a mask to reduce the chance of transmission. A two-day course of oral vitamin A is recommended for children with measles, although it does not prevent it.
My child has measles. What complications should I watch for?
Two important complications of measles are pneumonia (1 in 20) and brain swelling (encephalitis, 1 in 1000). Many cases of measles can safely recover at home, but you should seek immediate medical attention if your child is struggling to breathe or has altered mental status or seizures.
When should my child be immunized, and how effective is immunization?
Measles immunizations are usually given when children are one and four years old. Given Utah’s recent outbreak, infants 6-12 months old may receive an extra dose to get protection earlier. If you are interested in this, you can discuss it with your child’s physician.
The MMR immunization is 97% effective at preventing infection — only 4% of cases in 2025 were in immunized people. If your child is immunized and still gets measles, they will have a milder case and are less likely to have complications. If your child has not been immunized and you have concerns, please discuss them with your child’s physician.
What is subacute sclerosing panencephalitis (SSPE)?
SSPE is a complication of measles that can occur years after infection. One in 600 infants that get measles will have this complication, which is usually fatal, as was the case of a Los Angeles teenager who died from SSPE last year.
Is the MMR vaccine associated with autism?
No. Several large studies have been done to investigate this and immunized children have never shown an increased risk of autism.
How do the complications from the MMR vaccine compare to measles complications?
The table below describes possible complications and rates for both measles and the MMR vaccination. The MMR vaccination carries some side effects, but they pale in comparison to potential measles complications.
| Estimated risks for the MMR vaccine compared to risk of measles complications |
|---|
| MMR Vaccine Side Effects |
Fever, rash |
Swollen lymph nodes |
Joint pain |
Febrile seizure |
Immune Thrombocytopenic Purpura (ITP) |
I hope that through shared awareness, timely immunization and thoughtful public health action, we can reverse the spread of measles in our state and protect the youngest and most vulnerable among us.