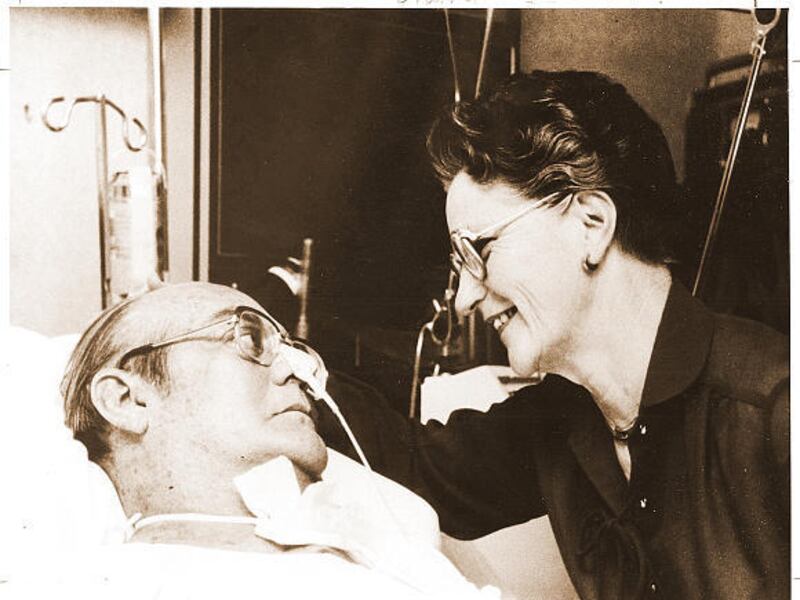
Countless calves and sheep, pounds of plastic and Dacron, miles of tubing, a hot tub and hundreds of bright minds and willing hands figuratively lined the road on which Barney Clark made his journey into medical history on Dec. 1, 1982 — as the first human to receive a total artificial heart, with FDA approval.
A quarter century has passed since a University of Utah team, led by Dr. William DeVries, implanted the Jarvik-7 artificial heart in the failing body of the Seattle dentist, so the anniversary is a fitting time to look at what led to the groundbreaking surgery and what has followed.
Later this week, U. officials and the Utah Artificial Heart Institute will host a two-day symposium at Huntsman Cancer Institute to mark the milestone. Many of the biggest names in heart repair — mechanical and medicinal — will gather Friday and Saturday to compare notes, celebrate Clark's legacy and discuss the future of cardiovascular treatment in a world where heart disease is the leading cause of death.
Barney Clark was born and educated in Provo, a Utah boy who moved to Seattle to study dentistry and stayed until the failure of his heart brought him back to seek care, first at LDS Hospital and later in the U.'s artificial heart program. He'd married UnaLoy Mason and they had three grown children, Stephen, Gary and Karen.
He consulted a young doctor at LDS Hospital, Jeffrey Anderson, now associate chief of cardiology at Intermountain Medical Center. LDS was just starting up a heart transplant program.
Initially, Clark was not a candidate for a human heart transplant. He was over 60 and had other medical problems. So Anderson managed his heart disease with medical therapy and clinical trials, "the latest and greatest at the time," he says today. That worked for a couple of years, then Clark began to fail rapidly.
About that time, Anderson had what he now calls a "key encounter in a hot tub" at the U. fieldhouse, where he and DeVries had each been working out. They chatted about the U's artificial heart program. Everyone knew by then that the U. was planning to implant someone; they were looking for the right candidate.
Anderson told DeVries about Clark, a man he recalls as "sophisticated medically and willing to be a guinea pig." Anderson sent Clark to see DeVries, and Clark's journey into history began.
"Barney was a real pioneer. He realized that with a first one, a lot can go wrong. He was willing to try," Anderson says.
Anderson was out of town when Clark's heart began the decline that would speed up the timeline for the historic surgery. He flew in during a mammoth snowstorm and went straight to the U., where he was also on the faculty, to watch the operation.
"Gosh, I wonder if this is going to make the local papers tomorrow," he remembers wondering.
Even in decline, Clark was a large man, about 200 pounds and over 6 feet tall, blessed with a chest that could accommodate what was a large, multichamber device.
He was also well-versed in the medical realities, aware that he would for his lifetime be tethered to mechanical out-of-body support by two, six-foot lines. It was hoped that with time that support would become more portable than the washer-size machine that powered his heart.
He was to be the first human recipient of a heart that had been used countless times in sheep and cows with funny names like "Tennyson" and "Abebe" and "Ted E. Bear," each with its own story.
One, Fernando, had three hearts, living 44 days on the Jarvik-7 before bridging to a transplant from his twin. He died 22 months later, not of complications from the hearts but from blood vessel problems caused by the repeated insertion of catheters to monitor his condition. Fernando proved that the mechanical heart could be a bridge to transplant — that the transplanted heart would grow with him.
Without the mechanical heart, Clark would die — a situation and requirement that was not negotiable for either the U.'s Institutional Review Board or the FDA when it came to implanting an unproven experimental device in a human.
Out of options, Clark had done his homework. He'd talked to numerous doctors, had intimate conversations with family members about their feelings, even visited the barns at the old St. Mark's Hospital on 800 South and 300 West to see the animals that walked on treadmills, artificial hearts pumping in their bovine chests. He'd signed the 11-page consent form once, then again a day later. And in the hours leading up to the surgery, he didn't waver, his widow, UnaLoy Farrer, says now.
"He wanted to help others who would come later. And he wanted to live."
In the years that have passed, many things have changed. Old collaborations have broken down, while others have strengthened. The ethical debates on use of the device have been replaced by new hot-button subjects, such as embryonic stem cells. Next-generation technologies that surely were rooted in the artificial heart, such as left-ventricular assist devices (LVADs), continue to save lives.
UnaLoy Farrer remembers the days surrounding the artificial heart transplant as a terrible, wonderful time.
Don B. Olsen, the veterinarian who had more experience than anyone implanting the device, albeit in livestock, calls it "a remarkable, fascinating time."
Cardiologist Anderson sees it as a "medical journey to the moon."
No one expected the international interest the 1982 surgery generated. "We thought we'd do our little experiment and then report the results," says Dr. Chase Peterson, then U. vice president over health services, who became the university's president later that year.
"If we'd said we were using an artificial gall bladder, we would probably not have had the same interest. There's something about the heart," says Peterson. Some of it was "probably not medical but poetic. 'With all my heart I love you.' 'We have to get to the heart of the matter.' It's a word used throughout civilization to describe the core of the human experience."
It was not the first artificial heart or even the first such instrument used in a human. Dr. Denton Cooley, a Texas heart surgeon, had twice implanted mechanical devices to help heart patients. One patient lived for a few hours after surgery. Many designs had been developed before Clark's artificial heart; his was the seventh design by Dr. Robert Jarvik, and Jarvik's efforts built on the many versions that had gone before that.
Dr. Willem Kolff, who ran the U.'s artificial heart program, is a storied name in the development of artificial organs. In Holland in 1943, he created an artificial kidney, the birth of dialysis, which today keeps thousands with failing kidneys alive.
Kolff immigrated to the United States, landing atthe Cleveland Clinic before the U. wooed him to head its program. Kolff himself, along with a colleague, placed an artificial heart in a dog in 1957. He brought with him to the U. two people, remembers Olsen, founder and president of the Utah Artificial Heart Institute, still located in the old hospital. Tom Kessler was a dental technician who was good at building and molding things, which made him an invaluable part of the artificial heart development team. The other was Dr. Clifford Kwan-Gett, a cardiovascular thoracic surgeon. Along with Kolff, they formed the nucleus upon which the U. built the artificial heart program and thus the heart that beat for 112 days in Clark's chest.
But in Kolff's program, improvements on an earlier version often led to a name change, "great motivation" for excellent work, in Kolff's book.
Jarvik's hearts built on work by Kwan-Gett, who'd had his name on earlier artificial hearts, as had others. Kwan-Gett's heart, which Olsen calls "a very, very good heart," included an innovation that has been used ever since. The device responded in animals to produce cardiac output. When cows implanted with it walked on a treadmill, the blood flow increased automatically.
That's a feature in the CardioWest heart, which has been implanted in more than 600 patients, usually as a bridge to human heart transplant. That heart came after the Jarvik-7, with slight modifications. In recent years, with its portable pneumatic driver, patients have survived an additional two years. Those who used it as a bridge to transplant have lived even longer.
Veterinarian Olsen was another core member of a team that over the years included hundreds of people. He was brought in first as a consultant in the late '60s, then hired to the team in the '70s because, at the time, "all the animals were dying."
He proved more versatile than imagined, even talking a mortgage company into donating the old hospital to the artificial heart effort. The team used St. Mark's old operating rooms on the top floor to implant devices in the animals. Olsen also proved to be a creative optimist. When a skeptic said that a pneumatic artificial heart would be defeated by atmospheric pressure, Olsen drove a sheep with an artificial heart to Snowbird and took pictures.
In the months following Clark's heart implant, surgical teams from around the world wanted to learn how to put the artificial heart into people. The FDA approved 27 teams, 23 of which Olsen says he personally trained, using calves as patients.
Five years after Clark's death, a total artificial heart was used for the first time as a bridge to transplant, implanted by Dr. Jack Copeland of Tucson, one of the bright lights coming to Utah this weekend.
Use of artificial heart technology has continued. LDS Hospital, for instance, implanted eight over the years, six of them as a temporary lifesaving bridge for patients awaiting human hearts.
Clark suffered perhaps more than anyone expected, with a heart malfunction at one point, seizures at another. His lung tissue was a mess, and bleeding and clots were major complications.
But he survived for three months.
"Before, we had some experience with cardiac support but had never removed a heart and never supported it for more than a day or two," Anderson says. "Clark's surgery showed you could support total cardiac function for an extended period of time."
Despite the complications, it was "revolutionary," he says.
The surgery was hotly debated: "Clark was too sick." "The device was not ready," critics said.
"But you have to at some point take a first step," Anderson says. "This was proof of principle."
"We were criticized for making a 'circus' out of the whole thing. That's the other side of being open. We thought we had to be open to avoid misconceptions," says Peterson. It was not like the experiments researchers do with mice.
That it involved a man, he says, made a huge difference.
"No one hovers around the mouse cage. This was an experiment of a different sort, and we were applauded and criticized. That's part of being a university," he says.
It was also a different time, medically speaking, says Dr. Edward "Mike" Gilbert, professor of medicine, director of the heart failure treatment program and medical director for heart transplants at the U.
In 1982, the medical arsenal against a failing heart was sparse — only a few centers were doing transplants, and medical management consisted primarily of digoxin, early oral vasodilator drugs and diuretics.
In the past 25 years, much has been learned about the activity of nerve and hormone systems in causing a weak heart to get larger and weaker. There have been hundreds of careful, prospective randomized trials to look at treatment outcomes, and multiple classes of medication have emerged, including beta blockers, ACE inhibitors and others.
Today, many people can be maintained for years with heart failure as a chronic condition. That wasn't the case back then. And electrophysiology — working with the heart's electrical system — is now possible, Gilbert says.
"Many people who either needed a heart transplant or total artificial heart are now successfully treated instead," he says, adding that when a transplant is done, there are better techniques and better immunosuppressant therapies, as well.
There is still a dearth, however, of donor hearts.
"It's still not a good disease, and the death rate is still pretty high with heart failure. But there's no question we've made good progress," Anderson says.
Today, stem cells offer hope of repairs for damaged heart tissue. It may be possible, Olsen thinks, to get stem cells to fix an area where heart cells have died. As to genetically engineering a heart itself, he's more skeptical. That requires specialized cells with electrical and circulatory capability and figuring out how to get cells to develop into valves. It's a very tall order.
The quest for ever-smaller, totally implantable, more perfect artificial hearts and heart-assist devices continues, but it is a "slow, but progressive" march, in Anderson's words. Jarvik later introduced a smaller, sleeker design; so have others. Several companies have their own iterations. The artificial heart is now both bridge and destination.
And it's a good bridge, Anderson says. As a destination therapy for those who will never get a transplant because they don't qualify, it's "pretty good for two years and better than the alternative, death." The infection rate is still a big problem, while clotting is less a problem than it was.
Innovation, too, has sparked technologies that provide backup support, like LVADs that help weak hearts rather than replacing them, sometimes even allowing a human heart to rest and heal. "Only in a few cases do you need a total artificial heart," he says.
Among the greatest innovations, says Gilbert, are the implantable defibrillator and the pacemaker.
LVADS are getting smaller and better. Anderson hopes he won't need one for a few years, if ever. But he's betting that in five years there will be one he is "comfortable putting in my family or myself, with a pretty good lifestyle."
Many researchers, including Olsen, continue to try to create the perfect artificial heart, eschewing parts that touch and wear out. He has learned from the breaking valves and malfunctioning diaphragms of earlier versions and is trying to make one that has neither problem. Like others, he wrestles with creating technology that prevents blood clotting. WorldHeart and MedQuest have both pursued designs based in part on his research and patents.
Since Clark died, animal hearts — including those of a pig, a baboon and later a genetically engineered pig heart with human blood — have been tried at least eight different times. But the emergence of latent viruses like mad cow disease makes Olsen think that the answer will not lie in an organ from another species.
Where will we be in another 25 years? the reporter asks.
"Further," she is told. There will likely be innovations not yet imagined. On that the experts agree.
E-mail: lois@desnews.com